by Dr. Mercola [1]
An estimated 15 to 20 million1,2 Americans use acid inhibiting drugs to treat heartburn. Indeed, PPIs are among the most widely prescribed drugs today, with annual sales of about $14 billion.3 This despite the fact that they were never intended to treat heartburn in the first place.
Research clearly shows that proton pump inhibitors (PPIs) are severely overprescribed and misused, and do far more harm than good in the long run. 4,5,6,7,8,9
If you suffer from frequent heartburn, rest assured there are many alternative treatment strategies that will help you eliminate this problem without serious side effects, which I’ll review toward the end of this article.
Beware: PPIs Are NOT Advisable for Majority of Heartburn Cases
Proton pump inhibitors like Nexium, Prilosec and Prevacid are actually designed to treat a very limited range of severe problems,10 including:
- Bleeding ulcers
- Zollinger-Ellison syndrome (a rare condition that causes your stomach to produce excess acid)
- Severe acid reflux, where an endoscopy has confirmed that your esophagus is damaged
These drugs were never intended for people with heartburn, and 90 to 95 percent of people taking them are not good candidates for these drugs. PPIs should also only be taken for a short period of time, yet many continue to take them for months or years on end.
PPIs Can Be Habit Forming and Dangerous
It’s important to realize that if you’re taking a PPI drug to treat your heartburn, you’re treating the symptom only; you’re not addressing the underlying cause, and by doing so, you’re exposing yourself to additional and potentially more dangerous health problems.
PPIs suppress the production of stomach acid, and contrary to popular belief, most cases of heartburn are actually due to having too little acid in your stomach, not too much. So taking a PPI will actually worsen your condition since stomach acid helps digest food protect against ingested pathogens.
Lack of stomach acid makes you more vulnerable to a number of problems, including nutritional deficiencies, food poisoning, and digestive system infections such as clostridium difficile.
Moreover, if you try to quit them cold turkey, your symptoms typically return with a vengeance. As noted by Marcella Lafayette, a 62-year-old heartburn patient interviewed by NPR:11
“I can’t seem to get off the drug, because when I do, I experience severe stomach pain. I can’t eat anything without experiencing stomach pain. It just feels like you’ve got a knife in your gut. It’s just really painful.”
How to Wean Off Your Heartburn Drugs
Since you can quickly develop both tolerance and dependence on these drugs, it’s important to wean yourself off them gradually to avoid severe rebound symptoms. NEVER stop taking proton pump inhibitors cold turkey.
To get off them, gradually lower the dose you’re taking while simultaneously implementing the recommended lifestyle modifications listed at the end of this article.
Once you get down to the lowest dose of the PPI, you can start substituting with an over-the-counter H2 blocker like Tagamet, Cimetidine, Zantac, or Ranitidine. Then gradually wean off the H2 blocker over the next several weeks.
PPIs Associated With Dementia and Other Serious Health Risks
Research has linked PPIs with a heightened risk for a number of serious health problems, including chronic kidney disease,12 pneumonia, osteoporosis [2], hip fractures, and dementia [3].
According to recent research13,14,15 published in JAMA Neurology, seniors over the age of 75 who use PPIs on a regular basis had a 44 percent increased risk of dementia, compared with nonusers. Men were at greater risk, raising their dementia risk on average by 52 percent, compared to 42 percent for women.
As noted by NPR:16
“How PPIs might increase the risk for dementia is unclear. But other researchers recently reported that, in the brains of mice, PPIs seem to increase levels of a damaging protein that accumulates in the brains of dementia patients, known as beta-amyloid.”
PPIs Linked to Heart Attack, Even in Those Without Cardiovascular Disease
Research has also linked long-term PPI use to an increased risk for heart disease17 and heart attacks [4].18,19,20 Disturbingly, your risk for a heart attack is increased even if you have no prior history of cardiovascular disease.
The reason for this effect is thought to be due to the drug reducing nitric oxide (NO) in your blood vessel walls. NO relaxes your blood vessels, so by reducing the amount of NO, PPIs may raise your risk of a heart attack.
To assess whether the use of PPIs were associated with a heightened cardiovascular risk among the general population, the team mined clinical data from more than 16 million medical records on 2.9 million patients.
This revealed that patients with gastroesophageal reflux disease (GERD) who took PPIs had a 16 percent increased risk of heart attack. Moreover, as reported by Scientific American:21
“Survival analysis in a prospective cohort found a two-fold increased risk of cardiovascular mortality in PPI users … H2 blockers, which include famotidine (Pepcid AC) and ranitidine (Zantac), were not associated with increased cardiovascular risk …
‘Consistent with our pre-clinical findings that PPIs may adversely impact vascular function, our data-mining study supports the association of PPI exposure with risk for MI in the general population,’ the authors write.”
Causes and First Line Treatments for Heartburn
“Heartburn,” also referred to as acid reflux, gastroesophageal reflux disease (GERD), or peptic ulcer disease, is characterized by a burning sensation originating behind your breastbone, sometimes traveling up into your throat. In some cases, this burning pain can be severe enough to be mistaken for a heart attack.
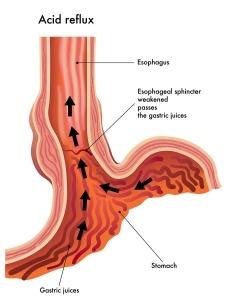
When food passes through your esophagus into your stomach, a muscular valve called the lower esophageal sphincter (LES) closes, preventing food or acid from moving back up.
The painful effect associated with heartburn occurs when the LES relaxes inappropriately, allowing acid from your stomach to flow (reflux) backward into your esophagus. While the conventional rationale states that this is caused by excessive amounts of acid in your stomach, that’s actually an extremely rare situation, typically occurring only if you have the rare condition known as Zollinger-Ellison syndrome.
The vast majority of acid reflux cases are in fact related to one or more of the following situations:
- Insufficient amounts of stomach acid. One simple strategy to address this deficiency is to swap out processed table salt for an unprocessed version like Himalayan salt. By consuming enough of the raw material, you will encourage your body to make sufficient amounts of hydrochloric acid (stomach acid) naturally.
Research22 has also shown that sauerkraut or cabbage juice is among the strongest stimulants for your body to produce stomach acid. It will also provide you with valuable bacteria to help balance and nourish your gut. Having a few teaspoons of fermented cabbage juice from sauerkraut before your meal will do wonders to improve your digestion. Fresh raw cabbage juice can also be very useful to heal resistant ulcers.
- Helicobacter pylori(H. pylori) imbalance. One of the explanations for why suppressing stomach acid is so ineffective — and there are over 16,000 articles in the medical literature attesting to this — is that when you decrease the amount of acid in your stomach, you suppress your body’s ability to kill the helicobacter bacteria.
While H. pylori can be part of your normal healthy microbiome, it can cause problems, including symptoms of acid reflux, if there’s an overgrowth of it. This typically occurs as a result of poor food choices.
Taking a betaine hydrochloric supplement (available in health food stores without prescription) will not only improve digestion, it will also help kill the helicobacter, thereby normalizing your symptoms. Other helpful foods and supplements known to suppress H. pylori are listed below.
- Hiatal hernia.23 If you have a hiatal hernia, physical therapy on the area may work, and many chiropractors are skilled in this adjustment.
- Food allergies can also be a contributing factor to acid reflux, so eliminate common culprits such as caffeine, alcohol [5], and nicotine.
Drug-Free Treatment Strategies
Ultimately, the answer to heartburn and acid indigestion is to restore your natural gastric balance and function and to do that, you need to address your gut health. The most important step is to eat real food, as processed foods and sugars are a surefire way to exacerbate acid reflux. Processed foods, especially sugar, also alter your gut microbiome and promote the overgrowth of harmful microbes. So be sure to eat lots of fresh vegetables and other unprocessed organic foods.
Reseeding your gut with beneficial bacteria, either from traditionally fermented foods [6] or a high-quality probiotic supplement is also important, as this will not only help balance your bowel flora, it can also help eliminate helicobacter bacteria naturally. Probiotics and fermented foods, especially fermented vegetables, also aid in proper digestion and assimilation of your food.
Other helpful strategies to get your heartburn under control [7] include the following suggestions, drawn from a variety of sources.24,25,26,27
- Raw, unfiltered apple cider vinegar – Acid reflux typically results from having too little acid in your stomach. You can easily improve the acid content of your stomach by taking one tablespoon of raw unfiltered apple cider vinegar [8] in a large glass of water.
- Betaine – Another option is to take a betaine hydrochloric supplement. You’ll want to take as many as you need to get the slightest burning sensation and then decrease by one capsule. This will help your body to better digest your food, and will also help kill the H. pylori bacteria.
- Baking soda – One-half to 1 full teaspoon of baking soda [9] (sodium bicarbonate) in an 8-ounce glass of water may ease the burn of acid reflux as it helps neutralize stomach acid. I would not recommend this as a regular solution but it can sure help in an emergency when you are in excruciating pain.
- Aloe juice – The juice of the aloe plant naturally helps reduce inflammation, which may ease symptoms of acid reflux. Drink about 1/2 cup of aloe vera juice before meals. If you want to avoid its laxative effect, look for a brand that has removed the laxative component.
- Ginger root – Ginger has been found to have a gastroprotective effect by blocking acid and suppressing helicobacter pylori.28 According to a 2007 study,29 it’s also far superior to lansoprazole for preventing the formation of ulcers, exhibiting six- to eight-fold greater potency over the drug. Add 2 or 3 slices of fresh ginger root to 2 cups of hot water. Let steep for about half an hour. Drink about 20 minutes or so before your meal.
- Vitamin D – Vitamin D is important for addressing any infectious component. Once your vitamin D levels [10] are optimized, you’re also going to optimize your production of about 200 antimicrobial peptides that will help your body eradicate any infection that shouldn’t be there. As I’ve discussed in many previous articles, you can increase your vitamin D levels through sensible sun exposure, a tanning bed, or an oral vitamin D3 supplement.
- Astaxanthin – This exceptionally potent antioxidant was found to reduce symptoms of acid reflux in patients when compared to a placebo, particularly in those with pronounced helicobacter pylori infection.30 Best results were obtained at a daily dose of 4 mg.
- Slippery elm – Slippery elm coats and soothes the mouth, throat, stomach, and intestines, and contains antioxidants that can help address inflammatory bowel conditions. It also stimulates nerve endings in your gastrointestinal tract. This helps increase mucus secretion, which protects your gastrointestinal tract against ulcers and excess acidity. The University of Maryland Medical Center 31 makes the following adult dosing recommendations: Tea: Pour 2 cups boiling water over 4 g (roughly 2 tablespoons) of powdered bark, then steep for 3 to 5 minutes. Drink 3 times per day. Tincture: 5 mL, 3 times per day. Capsules: 400 to 500 mg 3 to 4 times daily for 4 to 8 weeks. Take with a full glass of water. Lozenges: follow dosing instructions on label.
- Glutamine – Research32 published in 2009 found that gastrointestinal damage caused by H. pylori can be addressed with the amino acid glutamine, found in many foods, including beef, chicken, fish, eggs, dairy products and some fruits and vegetables. L-glutamine, the biologically active isomer of glutamine, is also widely available as a supplement.
- Folate or folic acid (vitamin B9) and other B vitamins – Research33 suggests B vitamins can reduce your risk for acid reflux. Higher folic acid intake was found to reduce acid reflux by approximately 40 percent. Low vitamin B2 and B6 levels were also linked to an increased risk for acid reflux. The best way to raise your folate levels is by eating folate-rich whole foods, such as liver, asparagus, spinach, okra, and beans.
- Melatonin, l-tryptophan, vitamin B6, folic acid, vitamin B12, methionine and betaine – A dietary supplement containing melatonin, l-tryptophan, vitamin B6, folic acid, vitamin B12, methionine and betaine, was found to be superior to the drug omeprazole in the treatment of GERD.34 Part of the success is thought to be due to melatonin’s inhibitory activity on nitric oxide biosynthesis, which plays an important role in transient lower esophageal sphincter (LES) relaxation, which, as I mentioned earlier, is part of the real underlying problem of GERD. Impressively, 100 percent of patients receiving this supplement reported a complete regression of symptoms after 40 days of treatment, compared to just under 66 percent of those taking omeprazole. The authors concluded that “this formulation promotes regression of GERD symptoms with no significant side effects.”
Tapping for Acid Reflux
Last but not least, you could even try the Emotional Freedom Techniques (EFT). In the video above, EFT practitioner Julie Schiffman demonstrates how to tap for acid reflux.
Sources and References
1, [11]11, [12]16 [13]NPR February 16, 2016 [14]
2 [15]Reuters June 10, 2015 [16]
3 [17]CBS News June 10, 2015 [18]
4 [19]Archives of Internal Medicine May 10, 2010; 170(9):784-90 [20]
5 [21]Archives of Internal Medicine May 10, 2010; 170(9):779-83 [22]
6 [23]Archives of Internal Medicine May 10, 2010; 170(9):772-8 [24]
7 [25]Archives of Internal Medicine May 10, 2010; 170(9):765-71 [26]
8 [27]Archives of Internal Medicine May 10, 2010;170(9):751-8 [28]
9 [29]CBS News December 27, 2011 [30]
10 [31]Archives of Internal Medicine 2010 May 10;170(9):747-8 [32]
12 [33]NPR January 12, 2016 [34]
13 [35]JAMA Neurology February 15, 2016, doi:10.1001/jamaneurol.2015.4791 [36]
14 [37]New York Times February 17, 2016 [38]
15 [39]Time February 16, 2016 [40]
17 [41]PLOS ONE December 27, 2013, DOI: 10.1371/journal.pone.0084890 [42]
18 [43]PLOS One June 10, 2015 [Epub ahead of print] [44]
19 [45]New York Times June 10, 2015 [46]
20, [47]21 [48]Scientific American June 10, 2015 [49]
22, [50]27 [51]Green Med Info Acid Reflux [52]
23 [53]WebMD Hiatus Hernia [54]
24 [55]Everydayroots.com, 15 Natural Remedies for Heartburn & Severe Acid Reflux [56]
25 [57]University of Maryland Medical Center, Slippery Elm [58]
26 [59]Science Daily May 22, 2009 [60]
28 [61]eCAM 2011, 2011:249487 [62]
29 [63]Molecular Nutrition & Food Research Mar 2007, 51(3):324-32 [64]
30 [65]Phytomedicine Jun 2008, 15(6-7):391-9 [66]
31 [67]University of Maryland Medical Center, Slippery Elm [58]
32 [68]Science Daily May 22, 2009 [60]
33 [69]Byron Richard’s Wellness Resources October 26, 2013 [70]
34 [71]Journal of Pineal Research Oct 2006, 41(3):195-200 [72]
Read the full article on Mercola.com [1]